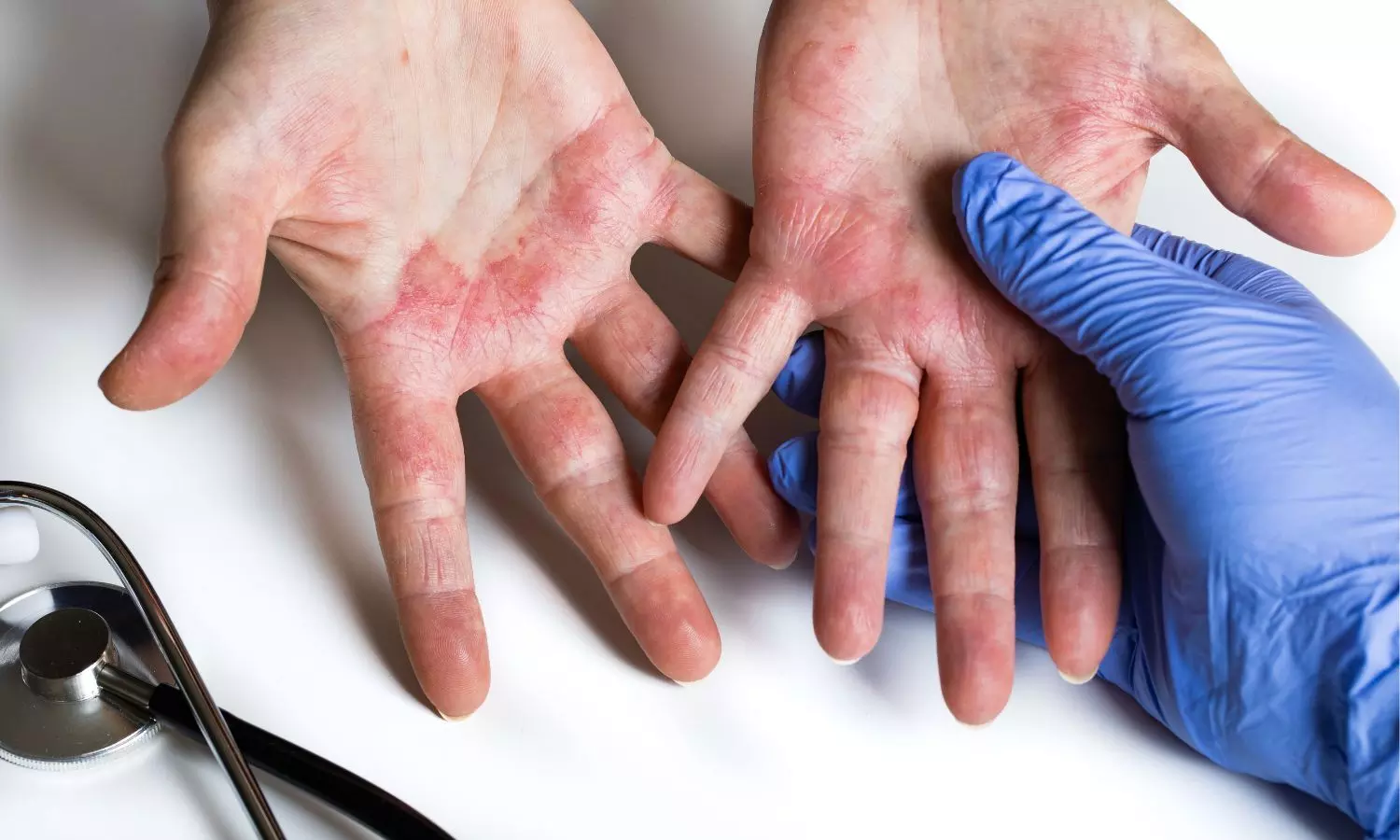
China: A recent case report published in Clinical, Cosmetic and Investigational Dermatology has highlighted how systemic contact dermatitis caused by benzalkonium chloride can be easily misdiagnosed as eczema, delaying appropriate treatment. The study, led by Man Yu from the Department of Dermatology, Hospital of Chengdu University of Traditional Chinese Medicine, China, highlights the importance of detailed exposure history in patients with persistent or treatment-resistant dermatitis.Allergic contact dermatitis (ACD) is a common inflammatory skin condition that often mimics other eczematous disorders, making diagnosis challenging. Benzalkonium chloride (BAK), a widely used compound found in disinfectants, preservatives, and household cleaning products, is increasingly recognized as a potential allergen. However, due to its widespread use, it is often overlooked as a trigger in clinical practice.The report describes a 31-year-old woman who presented with a two-month history of worsening skin symptoms, including widespread redness, scaling, intense itching, and localized discomfort. The lesions initially appeared in the lower back region and gradually spread symmetrically to the trunk and thighs. She had no history of fever, joint symptoms, or mucosal involvement.The patient had previously consulted multiple healthcare providers and was diagnosed with eczema and allergic dermatitis. She was treated with oral antihistamines and topical corticosteroids, which provided only temporary relief. Notably, her symptoms recurred quickly after stopping treatment, with each episode becoming more severe. She had no prior history of chronic illness, allergies, or exposure to new personal care products.Clinical examination revealed well-defined, erythematous, scaly plaques distributed mainly in areas in close contact with clothing, such as the waistline and lower torso. Laboratory investigations, including blood tests and autoimmune screening, were unremarkable. A skin biopsy showed features consistent with contact dermatitis, including mild spongiosis and superficial inflammatory infiltrates.A turning point in diagnosis came after a detailed reassessment of the patient’s environmental exposures. The patient reported recently using a new laundry disinfectant introduced approximately eight weeks before symptom onset. Further evaluation confirmed that the product contained benzalkonium chloride. Based on the temporal association, lesion distribution, and exclusion of other causes, a diagnosis of BAK-induced allergic contact dermatitis was established.The patient was treated with appropriate anti-inflammatory therapy and advised to completely avoid the offending product. Significant improvement was observed within two weeks, and complete resolution of symptoms was noted at one-month follow-up, confirming the causal relationship.The authors emphasized that such cases are not uncommon, as BAK-related dermatitis often resembles chronic eczema and may respond only transiently to standard therapies. They highlighted that laundry disinfectants are an underrecognized source of allergen exposure. The case also points to the need for clinicians to consider other similar compounds in household products that may provoke comparable reactions.Overall, the findings reinforce the critical role of thorough history-taking, particularly regarding household and environmental exposures, in patients with persistent dermatitis. Early identification and elimination of the causative allergen can lead to rapid recovery and prevent unnecessary prolonged treatment.Reference:Yu M, Meng F, Tian S. Systemic Contact Dermatitis Triggered by Benzalkonium Chloride in Laundry Detergent: A Case Initially Misdiagnosed as Eczema. Clin Cosmet Investig Dermatol. 2026;19:1-5https://doi.org/10.2147/CCID.S577154